GLP-1 and SGLT2 Drugs Found Safe From Serious Infection Risk in Major Global Study

A major global study has delivered reassuring news for millions of people who take GLP-1 receptor agonists and SGLT2 inhibitors for diabetes, weight loss, heart failure, and kidney disease. Researchers found that these widely prescribed medications do not significantly increase the risk of serious infections.
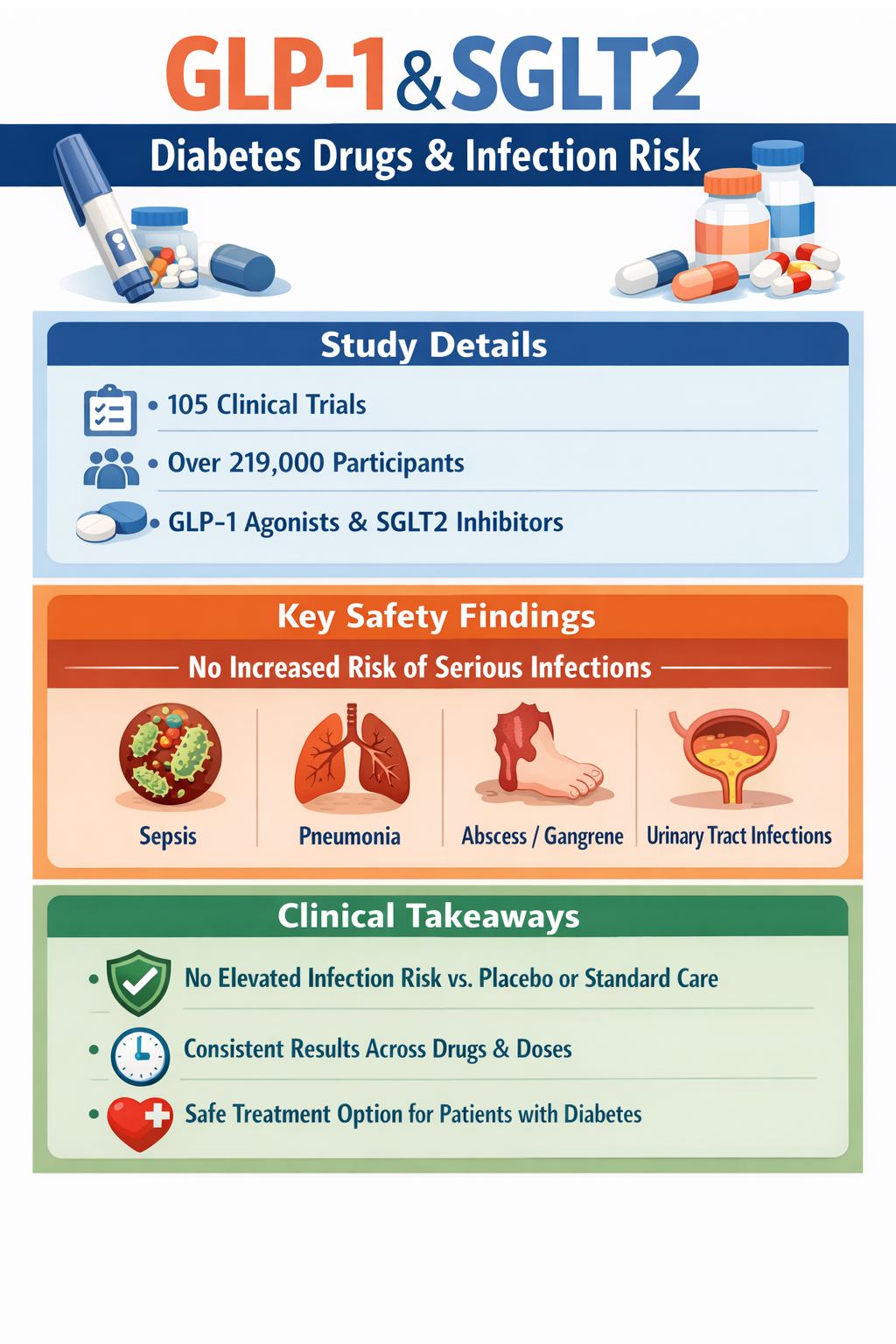
The finding comes from one of the largest analyses ever conducted on infection risk linked to these drugs. Scientists reviewed data from 105 randomized controlled trials involving 219,283 adults. They examined whether GLP-1 receptor agonists or SGLT2 inhibitors raised the risk of sepsis, abscess, gangrene, pneumonia, or urinary tract infections.
Their conclusion was clear. These medications do not meaningfully increase the risk of severe infections compared with placebo or standard treatment.
The question of infection risk has concerned doctors for years. People with diabetes already face a higher risk of infections because elevated blood sugar can weaken immune defenses. Excess glucose also creates an environment where bacteria thrive. Serious infections such as sepsis and soft tissue infections remain major causes of hospitalization and death in people with diabetes.
As prescriptions for GLP-1 drugs and SGLT2 inhibitors surged worldwide, clinicians wanted stronger safety data. Some earlier research suggested SGLT2 inhibitors could increase genital infections. Others raised questions about whether immune effects from these drugs might change vulnerability to serious infections.
To answer those concerns, researchers conducted a large network meta-analysis. This method allows scientists to compare multiple drugs and doses at the same time. The team searched major medical databases through December 18, 2024. They included only randomized controlled trials that reported infection-related outcomes.
Participants had no critical infection at the start of the trials. The researchers grouped infections into categories that included life-threatening sepsis, localized abscess or gangrene, and other infections such as pneumonia and urinary tract infections. They also examined treatment discontinuation rates to assess overall tolerability.
The results remained consistent across drug types and doses. Widely used GLP-1 receptor agonists such as semaglutide, liraglutide, dulaglutide, and tirzepatide showed no significant rise in severe infection risk. Common SGLT2 inhibitors including empagliflozin, dapagliflozin, ertugliflozin, and canagliflozin also showed no meaningful increase in sepsis or other major infections.
Researchers found no significant difference in rates of sepsis, abscess, gangrene, pneumonia, or urinary tract infections when comparing these medications with placebo or standard care. Longer treatment duration did not increase infection risk either.
One interesting finding emerged from the data. High-dose canagliflozin at 300 mg daily showed a statistically significant reduction in sepsis risk compared with control groups. Patients taking this higher dose appeared less likely to develop sepsis. However, when researchers removed one large clinical trial from the analysis, the protective effect lost statistical significance. That means the result should be interpreted with caution.
Aside from that isolated finding, no other drug or dosage showed a clear protective or harmful effect on serious infections.
The researchers strengthened their conclusions by following strict scientific standards. They registered their protocol in advance and adhered to recognized reporting guidelines. They used both frequentist and Bayesian statistical approaches to ensure robust results. Heterogeneity between studies was extremely low, which means findings were consistent across different populations and trial designs.
Subgroup analyses focusing only on patients with diabetes produced similar outcomes. Sensitivity testing confirmed that removing individual trials did not substantially alter the overall conclusions.
The timing of this research is significant. GLP-1 receptor agonists have become blockbuster therapies for both diabetes and obesity. Their benefits extend beyond blood sugar control. Many studies show these drugs reduce cardiovascular events and support meaningful weight loss.
SGLT2 inhibitors have also reshaped treatment guidelines. Doctors now prescribe them not only for diabetes but also for heart failure and chronic kidney disease. As their use expands beyond traditional diabetes care, understanding their safety profile becomes even more important.
For patients, the results offer reassurance. Individuals who qualify for GLP-1 or SGLT2 medications can feel more confident about their risk of developing serious infections while taking these therapies. Physicians can continue prescribing them without strong concern about triggering sepsis or major infection complications.
However, experts still urge careful monitoring. Diabetes itself remains a significant risk factor for infection. Maintaining good blood sugar control, practicing proper hygiene, and seeking medical care promptly for symptoms remain essential steps for patients.
Overall, this large-scale analysis fills an important knowledge gap in diabetes and cardiometabolic medicine. It provides strong evidence that GLP-1 receptor agonists and SGLT2 inhibitors do not significantly raise the risk of serious infections.
For millions of people managing diabetes, obesity, heart failure, or kidney disease, that conclusion brings welcome peace of mind.
References
Zeng, B. S., Chen, J. J., Hsu, C. W., Hung, C. M., Zeng, B. Y., Suen, M. W., … & Tseng, P. T. (2026). The Effect of GLP-1 Receptor Agonist and SGLT2 Inhibitor on Infection Risk: Network Meta-Analysis. Clinical Microbiology and Infection.
BMJ Rapid Review of SGLT-2 and GLP-1 Drugs
The BMJ. (2021). Sodium-glucose cotransporter-2 (SGLT-2) inhibitors and glucagon-like peptide-1 (GLP-1) receptor agonists for type 2 diabetes: systematic review and network meta-analysis of randomised controlled trials. BMJ, 372, m4573. https://www.bmj.com/content/372/bmj.m4573
Updated Living Systematic Review of Diabetes Medications
The BMJ. (2024). Medications for adults with type 2 diabetes: a living systematic review and network meta-analysis. BMJ, 390, e083039. https://www.bmj.com/content/390/bmj-2024-083039
Benefits and Harms of Antidiabetic Drugs
The BMJ. (2022). Benefits and harms of drug treatment for type 2 diabetes: systematic review and network meta-analysis. BMJ, 381, bmj-2022-074068. https://www.bmj.com/content/381/bmj-2022-074068
Network Meta-Analysis on Risk of Acute Kidney Injury
Hinduja, A., et al. (2021). Network meta-analysis of novel glucose-lowering drugs on risk of acute kidney injury. PubMed. https://pubmed.ncbi.nlm.nih.gov/33376101/
Efficacy and Safety of SGLT2 Inhibitors
Ma, G., & Li, Y. (2025). Efficacy and safety of 11 sodium-glucose cotransporter-2 inhibitors at different dosages in type 2 diabetes. BMJ Open, 15(2), e088687. https://bmjopen.bmj.com/content/15/2/e088687